In his book, Empire of the Scalpel, Ira Rutkow chronicles 4 main discoveries and victories that made the work of surgery the bliss we enjoy today.
“From medieval time to present day, successful practice of surgery anchored itself on 4 principal pillars: understanding of anatomy, control of bleeding, minimization of pain and minimization of the risk of infection…”
If I was to play a book critic, I would argue that optimizing lighting in the operating field is the masterstroke that the author did not spend his labour of love writing on.
“We are surgeons, not moles!” is a mantra those of us in the practice of surgery will resonate with. I have lifted the quotations from the seminal work of Abraham Verghese –Cutting for Stone . A shout of those words of displeasure indicates that it is time to adjust the overhead lighting to ensure the surgeon can properly see the operating field. “If you can’t see, I can’t see”, a surgeon I was assisting once bellowed at me. Now I find myself frequently repeating it to many an assistant.


The criticality of lighting in surgery may be best exemplified in minimal access surgery and endoscopic procedures. Here, lighting is everything. If lighting fails, you suspend the endoscopic procedure or convert it to open surgery. But when did the debate on lighting during open surgery take place? Who were the winners? I leave that for another day.
Unreliable Lighting in Rural Settings
For today, let me talk about the erratic and expensive power that we use. Again preaching to the choir? Yes, I thought so. After reading business opinion after business opinion on how domestic and commercial consumers in Kenya are ‘going green’ by turning to solar power with every rising sun, it is lost on no one that dependable power is a thorny issue.
Many hospitals in Rural Kenya may not be fully solar powered. And there’s always that occasional day when the back up generator may exhibit what a colleague in cardiology once dubbed ‘prolonged QR interval’: where the damn thing continues sleeping when it should have jumped out to save the world from the darkness ( I do not stand by the correctness of the parallelism between generator down time and those heart conduction problems, don’t quote me). It is those moments of darkness that may impact on a surgery, especially in demonstrating proper anatomy to enhance proper hemostasis (control of bleeding) on the table.
Lifebox has hence come up with a solution-a headlight- which is still at the experimental phase and I was happy to be gifted a set when I visited their stand in Windhoek, Namibia on the sidelines of the COSECSA conference. The amazing bit is that its battery is rechargeable. You just plug it to a USB charging port on your computer or use any of the ubiquitous charging plugs we use for our smart phones.. There is a another dry cell-powered battery in case you have to go without power for days. The black straps hold well on the head and the head light can zoom in and out creating varying sizes of the field of illumination, can adjust cephalocaudally ( well, I went to medical school to know another tongue twister for ‘up-and-down’) and select for different modes (warm vs daylight if you’re an electrician, open vs endoscopy light mode if you are a surgeon, white bright versus dim amber modes if you are neither of the above).



The first day I used it, it was on a total thyroidectomy or an open Nissen’s procedure, I can’t quite recall. I left theatre with a rye neck. That is my only concern- the weight of the gadget. Firstly, it makes one consciously aware that there is something on their heads. Secondly, the weight slowly adjusts the light beam out of focus on the operating field. On the one hour mark, I had to request an assistant to help re-focus.
After that initial experience, I kind of slowed down until I discovered the unspoken area of need for this light: the surgical ward procedure room. How many hospitals have ward procedure rooms? How well lit are those rooms? Over time, especially in the set up with private rooms, a bedside procedure may be preferably done in the patient’s room instead of in incurring the time, manpower and logistics of moving the patient to the corner procedure room and back.
Bedside Procedures and Clinical Examination
It was on a busy Tuesday afternoon when such was asked of me.
“Doc, the patient we saw needs a central line. The team is requesting for your help,” my intern called at a few minutes to 5 o’clock in the evening. I requested them to set sterile gloves, normal saline, local anesthetic and heparin besides the Central line kit.
“Can this bed go up?” I wondered loudly. We had set the bed against the window to allow in as much natural light as possible. But then we realized we had to draw the curtains to assure privacy around the general ward bed. I rushed back to the car and picked my box with the headlight. I always carry it in a bag with my scrubs, just incase. (I should add sterile gloves and tourniquet to that list. But hell no, I wont behave like that midwife I recently met who has a cord clamp as her car key holder). The team stared in amusement as I returned to the bedside assembling some black and red gadget.
” Local anaesthesia! Now the 10cc syringe and green needle!” the nurse kept handing these over while the intern assisted me fasten the battery in my pocket. We were done with the procedure in no time, getting the subclavian vein access with the first attempt and establishing good flows in all ports.
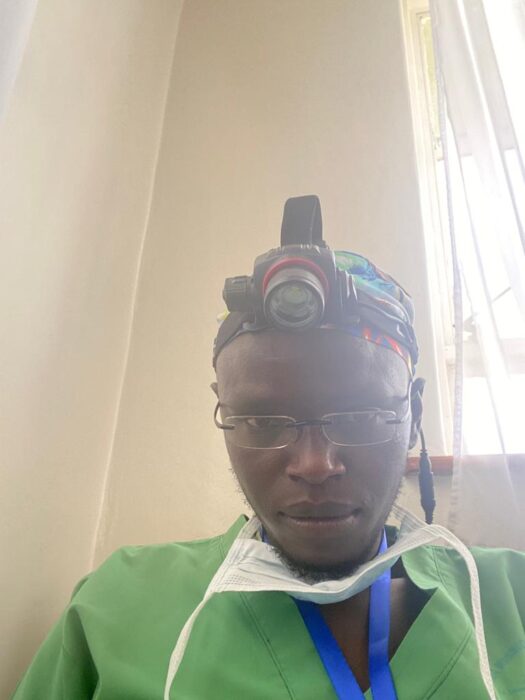
I look back and imagine how many junior colleagues will suffer in subcounty and smaller facilities where bedside procedures are needed but lighting is limited. It is simply too painful to countenance!
“I always put my chest tubes in theatre because of lighting and instruments”, a fellow general surgeon once told me. That is safe, I thought. But not many busy facilities will have the main theatre easily available for procedures that could be done at the bedside. And when it is easily available, it means the main theatre is not realizing its potential.
Besides general surgeons and general practitioners, Ear Nose and Throat (ENT) colleagues will find it even more useful. Whenever there is a black out at the clinic, this gadget saves the day. I know this from experience having lent my piece to a senior ENT surgeon when a power surge spoilt the headlight and the nearly 40 patients queuing outside had to contend with rumours of their clinic being cancelled.
“I can’t see any patient without the headlight”, my colleague stated matter of factly. He had to look inside the ears, the noses and/or the throats as his specialty demands, none of which areas renders itself to visibility using the ceiling lights.
“The biomed is already here but he says there is a piece that needs to be replaced”, the OPD manager confirmed when I called.
As a health executive, you quickly understand what such a statement means. It means that the unit in charge must raise the requisition order which will go to sectional finance head for signing then be handed over to the procurement. The procurement will raise a purchase order from this requisition. The purchase order will then go to the finance manager for signature before being forwarded to one of the C level executives for a final signature. The procurement officer will then use the fully signed purchase order to get one of the suppliers to supply the missing part. They will probably say ” we can deliver in a week”! Even in the event of emergency petty cash purchase, it might take you a whole day. Sometimes you will offer transport to go pick the item from the supplier then realize you have to wait for the driver who is already out of station dropping a group of staff for a scheduled seminar. Countless moving parts even with he best case scenario.
“Okay, I am coming”, I reassured the OPD manager as I got off my seat, picking my Lifebox headlight from the adjacent white cabinet where I had kept it in readiness for theatre. I passed by the ENT clinic enroute to main theatre. Even the spare light couldn’t be salvaged by the biomeds. Unfortunately for us, the ENT colleague had not carried along his personal headlight this day.
“Sorry about this doc. Let me hand you my portable headlight. You fix it like this, adjust it cephalo-caudally here, and you can use this to zoom”, I demonstrated. “Please disassemble it into this box once done and leave it with the OPD manager,” I left feeling like a magician. As I passed by the pool of patients waiting outside, I couldn’t help but notice the patients looking at me judgmentally imagining I was the long awaited biomed in-charge. Luckily for those with hearing impairments, alot of the indoor frustrations couldn’t be eavesdropped.
Now back to books critique. While I was in undergraduate training, I used to love this book by WHO titled Surgical Care at the District Hospital. If my memory serves me right, either there was a second volume or a chapter of the same volume titled “where there is no surgeon”. I can foresee the Lifebox headlight featuring in the future editions of the text carrying it’s own chapter- Where there is no Light.
I recommend this headlight to all colleagues working in resource limited facilities. I have shamelessly declared myself ‘The Village Surgeon‘ after working in rural Kenya for three quarters of a decade as a general surgeon. I know how handy this portable head light comes in. Therefore, if you operate in the rural areas of the global south, when there’s no light, try the lifebox head light.

